
Every pediatric emergency starts the same way. A child is in front of you, something is wrong, and you need to figure out what it is and act on it fast. The PALS Systematic Approach Algorithm gives you a structured, repeatable sequence to assess any critically ill or injured child, identify the most urgent problem, and intervene with the right treatment before the situation deteriorates further.
This algorithm is the foundation of everything in PALS. Before you can apply the cardiac arrest algorithm, the bradycardia algorithm, or the septic shock algorithm, you need to know what you are dealing with. The systematic approach is how you get there. It guides you from the first glance at the child through a full clinical assessment, so no critical finding gets missed, and no intervention gets delayed.

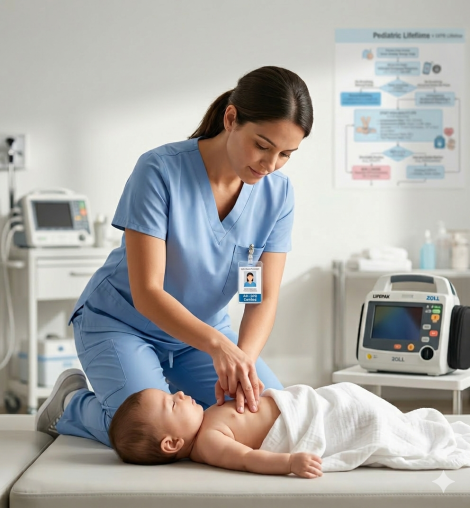

The PALS Systematic Approach Algorithm is the AHA-developed framework for assessing and managing any critically ill or injured pediatric patient. It applies to infants, children, and adolescents up to 18 years of age in any clinical setting, whether in the emergency department, intensive care unit, or prehospital environment. The algorithm does not target a specific condition. It is a universal assessment tool that guides you to the right diagnosis and the right intervention, regardless of the presenting problem.
The algorithm moves through three levels of assessment in sequence. The initial impression gives you a rapid, across-the-room read of how sick the child is. The primary assessment gives you a structured, hands-on evaluation of airway, breathing, circulation, neurological status, and exposure. The secondary assessment and diagnostic tests refine your clinical picture and confirm the underlying cause. At every stage, the algorithm directs you to intervene on any life-threatening finding before moving to the next level of assessment.
Unlike the other PALS algorithms, the systematic approach is not triggered by a specific rhythm or condition. It applies to every pediatric patient you encounter in a critical care setting. Interventions occur at every level whenever a life-threatening problem is identified. Do not wait until the full assessment is complete before acting. Below is the full step-by-step breakdown, starting from the moment you encounter a critically ill or injured pediatric patient.
The Pediatric Assessment Triangle (PAT) is the first tool you use in the PALS Systematic Approach. It takes seconds to complete and requires no equipment. The PAT provides an instant understanding of how sick the child is and which body system is most affected, all without you having to touch the patient. It has three components.
Appearance reflects the adequacy of oxygenation, ventilation, perfusion, and brain function. Assess tone, interactivity, consolability, gaze, and speech or cry. A child who is alert, interactive, and responding normally to their environment is less immediately concerning than a child who is limp, unresponsive, or inconsolable. Abnormal appearance is the strongest single indicator of a serious underlying problem.
Work of breathing reflects the child’s respiratory effort. Look for abnormal positioning like tripoding or sniffing. Listen for abnormal sounds such as stridor or grunting. Also check for retractions of the intercostal or suprasternal muscles and nasal flaring. Increased work of breathing indicates respiratory distress. In an unresponsive child, absent work of breathing indicates respiratory failure or arrest.
Circulation to the skin reflects the adequacy of cardiac output and perfusion. Assess skin color for pallor, mottling, or cyanosis. These findings indicate poor peripheral perfusion and reduced cardiac output. A child with normal skin color and tone is less likely to be in circulatory compromise than one who is pale, mottled, or cyanotic.
After completing the PAT, you have enough information to determine whether the child needs immediate life-saving intervention or can proceed to the primary assessment. If the child is in cardiopulmonary arrest, activate the emergency response system and begin CPR immediately. If the child is critically ill but not in arrest, move to Step 2.
The primary assessment is a rapid, hands-on evaluation of five physiological systems. It follows the ABCDE framework and identifies any immediate threats to life that require intervention before moving forward. Treat every life-threatening finding as you identify it. Do not complete the full assessment before intervening.
Assess whether the airway is patent, maintainable, or not maintainable. A child who is crying or speaking has a patent airway. Signs of obstruction include stridor, gurgling, abnormal positioning, or absent air movement. To open the airway, use a head tilt-chin lift. If you suspect a spinal injury, use a jaw thrust instead. Finally, insert an advanced airway if the airway cannot be maintained.
Assess respiratory rate, breath sounds, oxygen saturation, and work of breathing. Listen to both lung fields to check for equal air entry and abnormal sounds. A respiratory rate that is too fast, too slow, or absent requires immediate intervention. Provide supplemental oxygen, bag-mask ventilation, or advanced airway management based on the severity of the finding.
Assess heart rate, pulse quality, capillary refill time, skin temperature, and blood pressure. A heart rate outside the normal range for age, weak pulses, prolonged capillary refill greater than 2 seconds, and cool or mottled extremities all indicate circulatory compromise. Establish IV or IO access and initiate fluid resuscitation or vasoactive therapy based on findings.
Assess neurological status using the AVPU scale, which determines whether the child is Alert, responds to Voice, responds to Pain, or is Unresponsive. Check pupillary response and blood glucose immediately in any child with an altered mental status. If you detect hypoglycemia, you must correct it without delay to prevent further neurological compromise.
Remove clothing to inspect the full body for rashes, petechiae, trauma, surgical scars, and medical devices. After inspection, assess core body temperature and prevent heat loss by covering the child. Exposure findings often reveal the underlying cause of the emergency.
The secondary assessment follows the primary assessment once you have addressed immediate life threats. It consists of two components: a focused history and a focused physical examination.
The focused history follows the SAMPLE framework. You should gather information on Signs and symptoms, Allergies, Medications, Past medical history, Last oral intake, and Events leading to the current presentation. Since this information directly guides your differential diagnosis, you must speak to the parent or caregiver if the child cannot provide the history themselves.
The focused physical examination is a head-to-toe assessment that goes beyond the rapid ABCDE evaluation. Assess each body region systematically, looking for findings that were not identified during the primary assessment. Document all findings clearly and communicate them to the receiving team.
Diagnostic tests provide objective data to confirm your clinical findings and identify the underlying cause of the emergency. Order tests based on the most likely diagnosis identified during the primary and secondary assessments. Do not delay life-saving interventions while waiting for results.
Common diagnostic tests in the PALS Systematic Approach include a 12-lead ECG to identify rhythm and conduction abnormalities and chest imaging to evaluate respiratory and cardiac pathology. You should obtain point-of-care glucose immediately for any child with an altered mental status and use arterial or venous blood gases to assess oxygenation and ventilation status. A complete blood count and metabolic panel are essential for identifying infection and electrolyte abnormalities. At the same time, point-of-care ultrasound should be used to evaluate cardiac function and fluid status in real time.
Once your assessment is complete, identify the primary problem driving the child’s clinical deterioration. In PALS, problems fall into four categories, which include respiratory problems, circulatory problems, cardiopulmonary failure, and cardiac arrest. Cardiopulmonary failure, the combination of respiratory failure and circulatory shock occurring simultaneously, represents a pre-arrest state requiring immediate aggressive intervention.
Select the appropriate intervention based on your identified problem. General interventions apply to all critically ill children, which include oxygen delivery, vascular access, cardiac monitoring, and fluid resuscitation. You must then target specific interventions to the identified problem, such as using bronchodilators for bronchospasm or synchronized cardioversion for unstable tachycardia. If cardiac arrest is identified, activate the Pediatric Cardiac Arrest Algorithm immediately.
After every intervention, reassess the patient immediately. Do not assume an intervention worked without confirming it. You should check whether the child’s airway, breathing, circulation, and neurological status have improved, remained the same, or deteriorated to determine your next steps. A child who improves is responding to treatment, while a child who does not improve or continues to deteriorate requires a different intervention or an escalation of care. This reassessment restarts the Evaluate-Identify-Intervene sequence and continues until the child is stable or a specific PALS algorithm is activated.
The Evaluate-Identify-Intervene sequence is the core clinical cycle that drives the PALS Systematic Approach Algorithm. It is not a one-time process. It repeats continuously throughout the resuscitation until the child is stable.
Evaluate means assessing the child using the tools covered in the algorithm steps, starting with the PAT, moving through the ABCDE primary assessment, and refining your picture with the secondary assessment and diagnostic tests.
Identify means naming the specific problem driving the child’s deterioration. Identifying the problem correctly determines which intervention you select. A wrong identification leads to a wrong intervention, which wastes time and worsens outcomes.
Intervene means acting on the identified problem without delay. General and specific interventions are applied based on the clinical findings. Every intervention is followed immediately by reassessment.
The cycle then restarts. This continuous loop of evaluating, identifying, and intervening is what keeps a deteriorating child from progressing to cardiac arrest. It is what separates a structured clinical response from a reactive one.
The PALS Systematic Approach Algorithm is not a standalone protocol. It is the entry point for every other algorithm in the PALS framework. The problem you identify in Step 5 determines which algorithm you activate next.
Here is how each clinical finding connects to the corresponding PALS algorithm:
Understanding how the systematic approach feeds into each algorithm is what allows a PALS provider to move from assessment to treatment without hesitation. The systematic approach identifies the problem. The specific algorithm tells you exactly what to do about it.
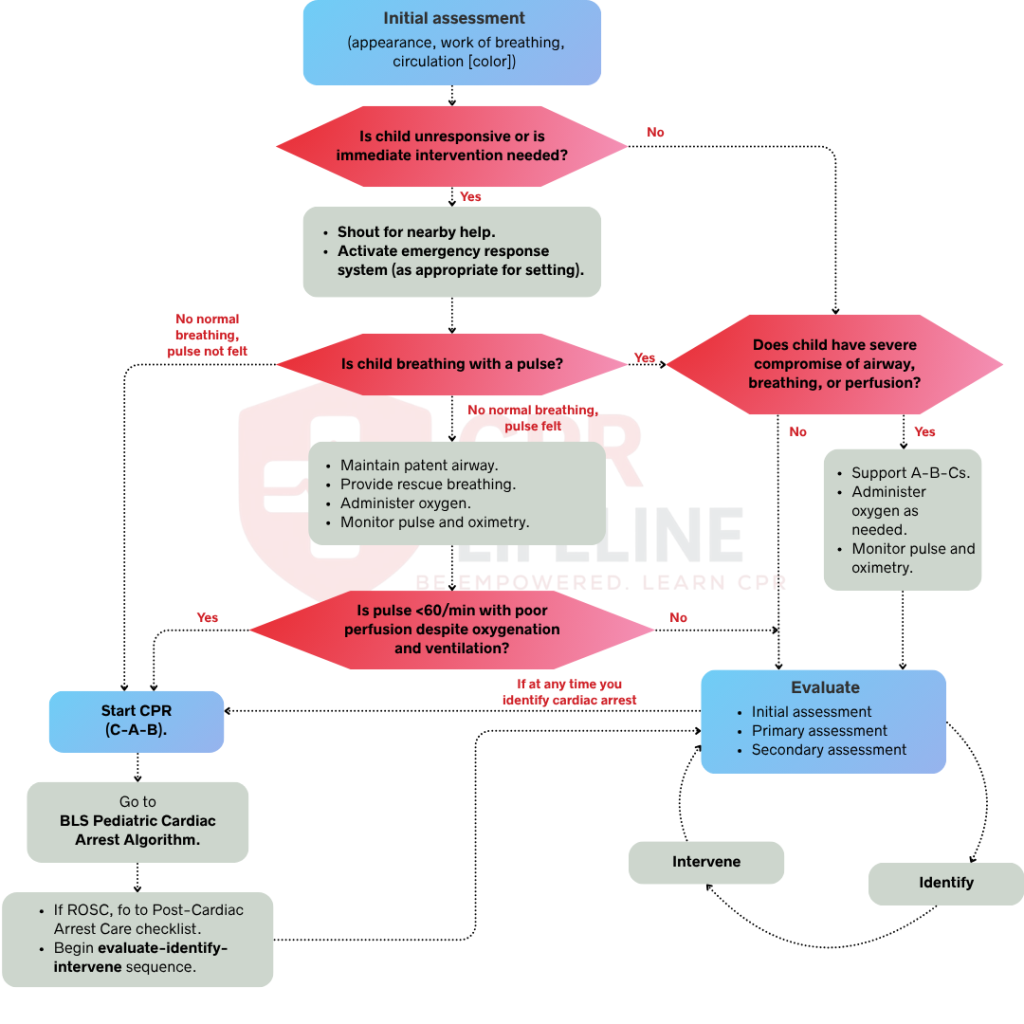
Reading through the PALS Systematic Approach Algorithm builds essential familiarity with the assessment sequence. Applying it correctly under pressure during a real pediatric emergency is an entirely different skill. The PAT, the ABCDE assessment, and the Evaluate-Identify-Intervene cycle all require repetition in a simulated clinical environment before they become automatic.
Building that competency requires hands-on simulation in a structured setting. If you are preparing for initial PALS certification or an upcoming recertification, CPR Lifeline offers AHA-authorized PALS courses. These courses include pediatric-specific simulations that cover every algorithm, including the systematic approach.
By submitting this form you agree to receive text messages at the provided number from CPR Lifeline LLC for appointment reminders. Message frequency varies, and standard message and data rates may apply. You have the right to OPT-OUT of receiving messages at any time. To OPT-OUT, reply “STOP” to any text message you receive from us. Reply HELP for assistance.
The 3 components of the Pediatric Assessment Triangle are appearance, work of breathing, and circulation to the skin. Appearance reflects oxygenation, perfusion, and brain function. Work of breathing reflects respiratory effort and distress. Circulation to the skin reflects cardiac output and peripheral perfusion. The PAT requires no equipment and takes seconds to complete.
The Evaluate-Identify-Intervene sequence is the core clinical cycle of the PALS Systematic Approach. Evaluate means assessing the patient using the PAT, primary assessment, secondary assessment, and diagnostic tests. Identify means naming the specific problem driving deterioration. Intervene means acting on that problem without delay. The sequence repeats continuously after every intervention until the child is stable.
The 4 problem categories are respiratory problems, circulatory problems, cardiopulmonary failure, and cardiac arrest. Respiratory problems include respiratory distress and failure. Circulatory problems include compensated and decompensated shock. Cardiopulmonary failure is the combination of respiratory failure and circulatory shock occurring simultaneously and represents a pre-arrest state. Cardiac arrest requires immediate CPR and activation of the Pediatric Cardiac Arrest Algorithm.
The primary assessment is a rapid, hands-on ABCDE evaluation that identifies immediate life threats requiring intervention. It is performed first, and treatment begins as life-threatening findings are identified. The secondary assessment follows once immediate threats are addressed. It consists of a focused history using the SAMPLE framework and a focused physical examination to identify the underlying cause of the emergency.
Activate the Pediatric Cardiac Arrest Algorithm immediately when the child is unresponsive with no breathing or only gasping, or when the pulse is absent or below 60 beats per minute with signs of poor perfusion despite adequate oxygenation and ventilation. Do not continue the systematic approach when cardiac arrest is identified. Begin CPR without delay and transition to the Cardiac Arrest Algorithm.
AVPU stands for Alert, Voice, Pain, and Unresponsive. It is a rapid neurological assessment tool used during the disability component of the ABCDE primary assessment. Alert means the child is awake and aware. Voice means the child responds to verbal stimulation. Pain means the child only responds to painful stimuli. Unresponsive means the child has no response to any stimulation and requires immediate intervention.
Home | About Us | Classes | Locations | Blogs | FAQ’s | Group Training | Contact Us
#1. Select your Course, Location and Time
#2. Complete the AHA Online Training
#3. Perform the hands on skills check
#4. CONGRATS! You are certified!