
Cardiac arrest can happen without warning to anyone. You may be the only person present when it happens. The Adult BLS Algorithm for Lay Rescuers gives you a simple, evidence-based sequence to follow until professional help arrives. The American Heart Association updated this algorithm in 2025 to make it easier for everyday people to act quickly and effectively.
Every second without intervention reduces the chance of survival. This version focuses on rapid recognition and immediate action. Untrained rescuers start with hands-only CPR, but trained rescuers who are willing can add rescue breaths. The algorithm also guides you to use an AED as soon as one is available and to give naloxone if you suspect an opioid overdose. Performing these steps without hesitation can keep blood flowing to the brain and heart in those first critical minutes.

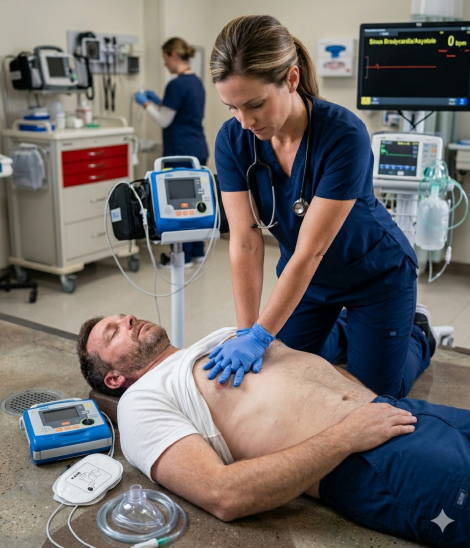

The Adult BLS Algorithm for Lay Rescuers is the American Heart Association’s simplified protocol for anyone who witnesses a sudden cardiac arrest in an adult. It applies to both untrained and trained lay rescuers. The algorithm focuses on rapid recognition of unresponsiveness and abnormal breathing, immediate activation of emergency services, high-quality chest compressions, and early use of an AED.
You do not need advanced medical training to follow this sequence. The 2025 update emphasizes hands-only CPR as the default for most lay rescuers. Trained rescuers who feel comfortable may add rescue breaths in a 30:2 ratio. The algorithm also includes guidance on giving naloxone when you suspect an opioid overdose. Every step is designed to maintain blood flow to the brain and heart until professional rescuers take over. Quick action using this sequence greatly improves the victim’s chance of survival with good neurological function.
The Adult BLS Algorithm for Lay Rescuers follows a simple sequence, which is designed to be simple, fast, and actionable. You can perform some actions at the same time when more than one person is present. Follow the steps exactly as shown. Quick action improves the victim’s chance of survival.
Tap the person firmly on the shoulders and shout, “Are you okay?” loud enough for them to hear. Look for any response, including movement, sound, or eye opening. At the same time, look at the chest for normal breathing. Gasping or no breathing at all confirms the person needs help. The 2025 AHA guidelines do not require lay rescuers to perform a pulse check, as accurate pulse detection is unreliable without training. If the person is unresponsive and not breathing normally, treat it as a cardiac arrest and move immediately to the next step.
Call 911 immediately or point to one person and say, “You, call 911 now,” to prevent the bystander effect. At the same time, send another bystander to find the nearest AED. If you are alone, call 911 yourself before starting CPR. Put the call on speaker so you can follow dispatcher instructions while keeping your hands free. Do not leave the patient unattended any longer than necessary.
If an AED is nearby and retrievable within seconds, get it first before starting CPR. If it requires leaving the patient for more than a few seconds, start CPR immediately and have someone else retrieve it. The AED should be obtained and ready to use as quickly as possible without interrupting chest compressions.
Begin chest compressions immediately after calling for help. Place the heel of your dominant hand on the center of the chest, directly on the lower half of the breastbone. Place your other hand on top and interlace your fingers. Keep your arms straight and position your shoulders directly over your hands. Compress hard and fast at a rate of 100 to 120 compressions per minute. Allow the chest to fully rise between each compression without leaning on it.
If you have no CPR training or are not comfortable giving breaths, perform hands-only CPR. Push hard and fast on the center of the chest and do not stop until EMS arrives or someone with more training takes over. Hands-only CPR is highly effective and significantly better than doing nothing. Do not stop to check for a pulse or a response during CPR unless the person starts breathing normally or moving on their own.
If you are trained in CPR and willing to give breaths, use a 30:2 ratio. Deliver 30 chest compressions followed by 2 rescue breaths. To give a breath, tilt the head back, lift the chin, pinch the nose, and seal your mouth over the person’s mouth. Each breath should last one second and produce a visible chest rise. If the chest does not rise, reposition the head and try once more before returning to compressions. Do not pause compressions for more than 10 seconds to give breaths.
As soon as the AED is available, turn it on and follow the audio prompts. Attach the pads to the person’s bare, dry chest. Place one pad below the right collarbone and the other on the left side of the chest below the armpit. Stop CPR only while the AED analyzes the rhythm and delivers a shock. Resume compressions immediately after each shock without waiting to check for a pulse.
If the AED advises a shock, make sure no one is touching the patient and then deliver the shock. Immediately resume CPR after the shock. Keep repeating the cycle of two minutes of CPR followed by AED analysis until EMS arrives, the person starts breathing normally, or you are physically unable to continue.
If the AED advises no shock, resume CPR immediately without delay. A non-shockable rhythm means defibrillation will not help, but high-quality chest compressions remain the most important intervention. Continue CPR and follow AED prompts every two minutes until EMS arrives.
High-quality CPR is an important factor in cardiac arrest survival. Performing the steps is not enough. How well you perform them determines whether an adequate amount of blood reaches the brain. These are the standards every lay rescuer should know.
Compress at a rate of 100 to 120 per minute and to a depth of at least 2 inches but no more than 2.4 inches. Push using your body weight rather than your arm strength, while keeping your arms straight and your shoulders directly over your hands. If you are unsure of the rate, compress to the beat of a song with approximately 100 to 120 beats per minute.
Allow the chest to return completely to its natural position between each compression. Do not lean on the chest between compressions, as it reduces blood flow to the heart. Fatigue is the most common cause of poor recoil. If multiple bystanders are present, rotate the compressor role every two minutes to maintain the quality of resuscitation.
Every pause in chest compressions reduces blood flow to the brain. All the interruptions must be kept under 10 seconds. Do not pause to check for a pulse or a response unless the person starts breathing normally or moving. The only acceptable reasons to pause are AED analysis, shock delivery, and giving rescue breaths in a 30:2 ratio.
Some cardiac arrest situations require a slightly different response. Knowing these variations before you need them ensures you act correctly without hesitation in emergency situations.
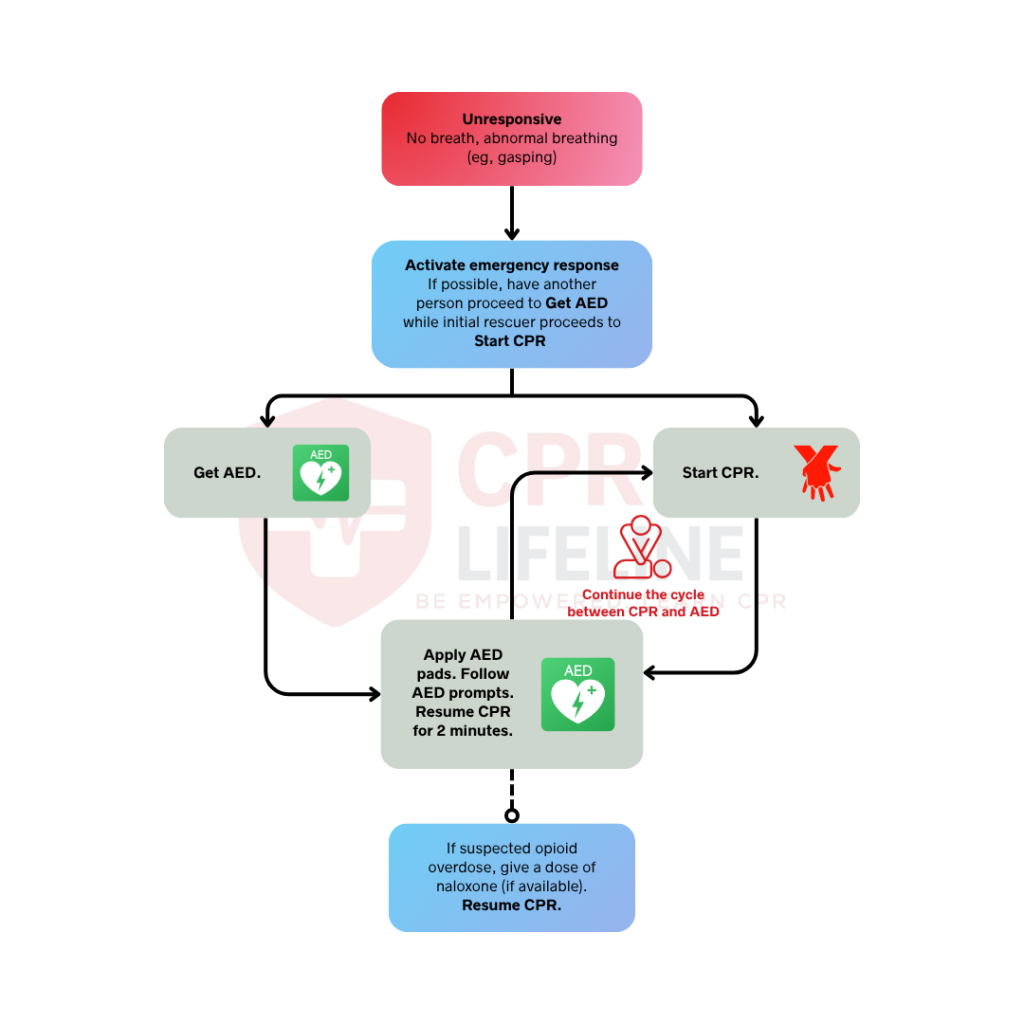
The Adult BLS Algorithm for Lay Rescuers provides a clear framework for responding to cardiac arrest. By focusing on rapid recognition and high-quality chest compressions, this protocol ensures that bystanders can make a difference. Whether you perform hands-only CPR or provide rescue breaths, the goal is to keep oxygenated blood flowing to the brain. Practicing these steps is essential because acting without hesitation becomes the most critical link in the chain of survival.
Mastering these skills requires hands-on practice to ensure your technique meets modern standards. CPR Lifeline offers an AHA authorized BLS course that provides the confidence and practical experience needed for real-world emergencies. Enrolling in a course at CPR Lifeline prepares you to apply the 2025 guidelines with precision when every second counts.
By submitting this form you agree to receive text messages at the provided number from CPR Lifeline LLC for appointment reminders. Message frequency varies, and standard message and data rates may apply. You have the right to OPT-OUT of receiving messages at any time. To OPT-OUT, reply “STOP” to any text message you receive from us. Reply HELP for assistance.
The 2025 AHA guidelines do not require lay rescuers to check for a pulse. Many people find it difficult to locate a pulse quickly during an emergency. If the person is unresponsive and not breathing normally, you should assume cardiac arrest and start compressions immediately.
Hands-only CPR consists of continuous chest compressions without rescue breaths and is the standard for untrained rescuers. Traditional CPR involves a cycle of 30 compressions followed by 2 breaths. Both methods are effective, but hands-only CPR is often easier for bystanders to perform correctly under pressure.
Most regions have Good Samaritan laws that protect bystanders who act in good faith to provide emergency assistance. These laws are designed to encourage people to help without the fear of legal consequences. Your quick intervention is much better than doing nothing at all.
It is common for ribs to crack or for the chest to make popping sounds during high-quality compressions. If this happens, do not stop or reduce your force. Proper depth is necessary to move blood to the brain, and any skeletal damage can be treated after the person is resuscitated.
You will not know immediately if a shock has restored a normal heart rhythm. This is why the algorithm directs you to resume chest compressions the moment a shock is delivered. The AED will re-analyze the heart rhythm every two minutes and provide further instructions.
Yes, an AED is safe and recommended for use on pregnant patients in cardiac arrest. The procedure remains the same as it would for any other adult. Saving the mother is the best way to save the baby, so you should follow the AED prompts without delay.
You should continue CPR until the person starts to breathe or move, the AED instructs you to pause for analysis, or professional EMS providers take over. You may also stop if the scene becomes unsafe or if you become too physically exhausted to continue.
Home | About Us | Classes | Locations | Blogs | FAQ’s | Group Training | Contact Us
#1. Select your Course, Location and Time
#2. Complete the AHA Online Training
#3. Perform the hands on skills check
#4. CONGRATS! You are certified!